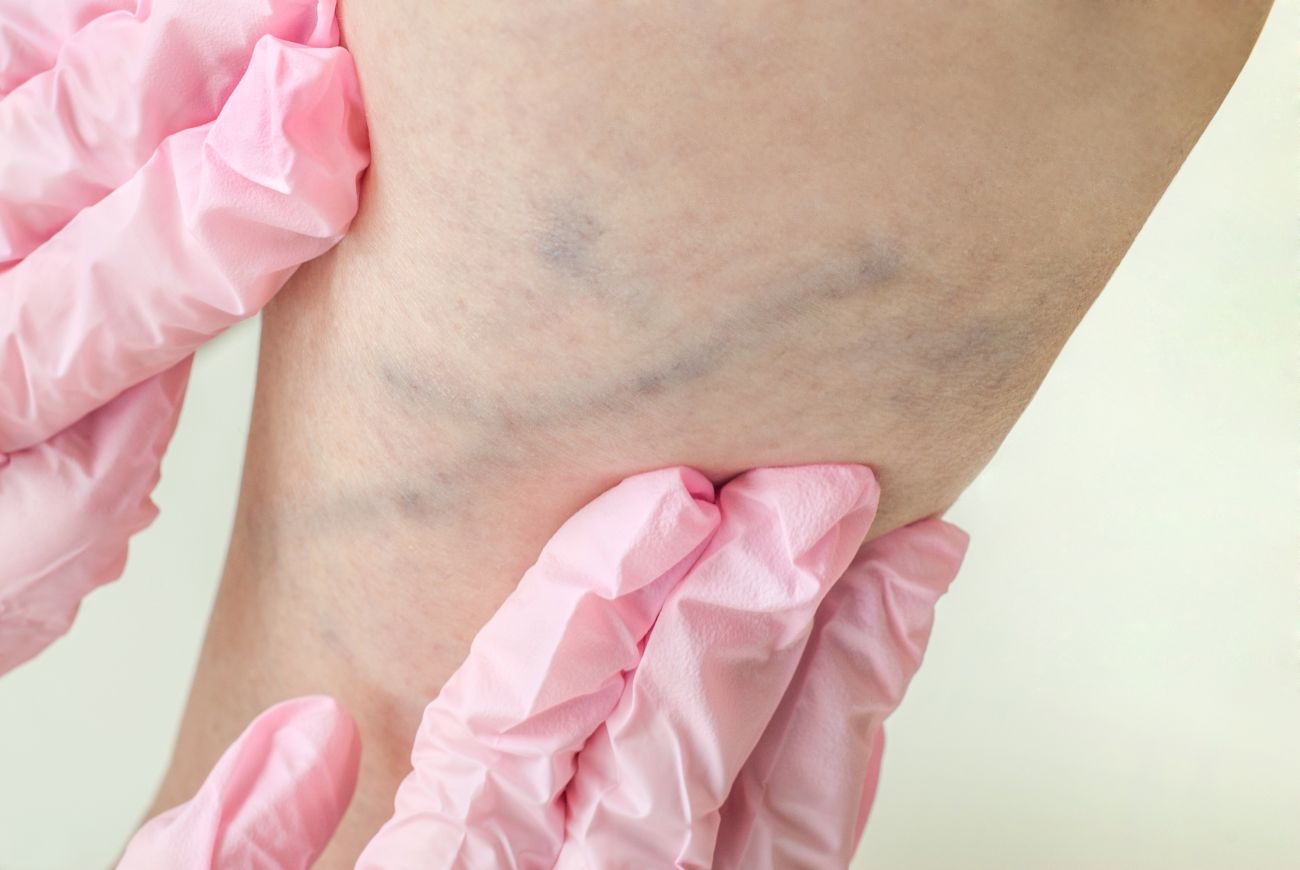
Deep Vein Thrombosis, commonly known as DVT, is a type of blood clot that forms within a deep vein in the body. The majority of the DVT clots occur in the thigh vein or lower leg vein.
DVT is a serious and potentially life-threatening condition that gets complicated when the clot disengages from the deep vein and travels into the lungs. This condition is known as pulmonary embolism (PE).
Together, DVT and PE are collectively termed as Venous Thromboembolism (VTE).
Dangers of Deep Vein Thrombosis
According to the Centers for Disease Control and Prevention (CDC), VTE affects approximately 900,000 Americans every year. Moreover, about 60,000 to 100,000 people in the U.S. die from blood clots every year.
And this isn’t all. In fact, the CDC estimates one in every four people are likely to die suddenly from PE.
But there is some good news: DVT is preventable. Through the right education and timely diagnosis, DVT-related disease complications can be avoided.
Signs and Symptoms
Deep vein clots mostly form in the thighs or lower leg. Sometimes, they may also form in the arm.
The most common symptoms of DVT are:
- Extreme swelling on the affected leg or arm;
- Cramping pain around the affected leg or arm that radiates from calf to leg or from arm to forearm;
- Swollen part of the affected arm or leg appears warm, and;
- The skin around the affected area usually turns pale, reddish, or bluish in color.
Surprisingly, not all people with DVT experience symptoms.
Causes
DVT is a form of a blood clot that disrupts normal blood circulation in your body. It can occur due to several reasons. The most common causes behind DVT formation are:
- Injury,
- Surgery,
- Inactive lifestyle, and
- Use of certain medications.
Injury
Deep injuries can damage the structure of blood vessels. This damage causes them to shrink and block normal blood flow, which results in a blood clot.
Surgery
Much like deep injuries, surgeries can directly damage blood vessels and cause a blood clot.
Inactive Lifestyle
Another cause of DVT comes from a sedentary lifestyle. People who are inactive and less mobile are more likely to get blood clots. Sitting for prolonged periods disrupts normal blood flow. This inactivity causes the blood to pool down around a spot, thus increasing the chance of clot formation.
This is why DVT is common in hospitalized, paralyzed, and bed-ridden patients. It’s even common in frequent travelers who spend several hours sitting in planes, trains, and cars.
Use of Certain Medications
The use of certain medications, such as contraceptive pills, is associated with clot formation and DVT.
Other Factors
Other factors that can lead to DVT include:
- Smoking;
- Obesity;
- Presence of diseases like cancer, and;
- Heart failure.
Diagnosis
The diagnosis of DVT includes a physical examination and a simple ultrasound scan to visualize blood flow through veins of the affected part. In the presence of a suspected clot, an X-ray of the clotted vein is performed to pinpoint the exact location of the blood clot.
However, the problem with the ultrasound scan is that it might produce a false positive or false negative, providing a need for other assessment tools to diagnose the disease better. One such scoring system is the Wells criteria, which is widely used across the U.S.
Treatments
DVT is a serious and potentially fatal condition that requires prompt treatment and management. Once an accurate diagnosis is made, several measures are taken to remove the clot, prevent it from growing and causing a pulmonary embolism, and to reduce the risk of having more clots in the future.
Medication
Blood thinners or anticoagulants are the most commonly used to treat DVT. By thinning blood, these medications improve blood flow and prevent blood clots from growing further. Blood thinners also prevent the formation of new clots.
In more severe cases, fibrinolytic drugs may be used. These medications essentially destroy blood clots by breaking them down. Fibrinolytics are given through IV injections.
Filters
In cases when a DVT patient cannot take blood thinners or fibrinolytics, filters might be used as a short-term treatment to prevent clots from entering the lungs. Filters are inserted into a large vein in the patient’s stomach from where they stop the existing clots from making their way into the lungs.
Surgery
In more severe cases of DVT, when multiple large clots are formed and the patient is unable to tolerate blood thinners, surgery might be the last resort to prevent tissue damage and other complications. The procedure involves making an incision into the affected blood vessel, removing the clot physically, and repairing the blood vessel.
An alternative method involves using a catheter that keeps the blood vessel’s diameter open while the surgeon removes the clot. Once the clot is pulled out, the catheter is removed.
Compression Stockings
People at high-risk for DVT need to take adequate measures to prevent the clot from forming in the first place. Wearing compression stockings is a great way to avoid clot formation and reduce swelling.
In fact, a 2016 study published in the Cochrane Database of Systematic Reviews suggested that compression stockings can lower the risk of DVT in airline passengers.
Physical Exercise
Sitting for more extended periods disrupts normal blood flow and increases the risk for DVT. Therefore, it is best advised to stay active, walk regularly, and perform a bunch of exercises to keep legs mobile and promote adequate blood flow.
One effective way to prevent blood from pooling down into lower or upper extremities is keeping legs and arms elevated whenever possible. Placing legs at a level parallel to hips does wonders in preventing blood from accumulating into the legs.
Living with Deep Vein Thrombosis
DVT is a serious health condition that can develop into a life-threatening illness. Together, DVT and PE constitute VTE, which is the third leading cause of cardiovascular death worldwide.
While there is no cure to the disease, living with DVT isn’t as challenging as it sounds. With an appropriate diagnosis, prompt management, and some lifestyle modification, people with DVT can lead a healthy life.